 Repeat tuberculin tests have been reported to accentuate the response in persons with active or latent tuberculosis infection. However, the accentuating effect of BCG on the tuberculin test wanes after vaccination 1 and is extremely unlikely to be responsible for severe bulla formation 10 years later. The BCG vaccination might result in false-positive results in tuberculin tests. She had undergone BCG vaccination, which is routine for all newborn babies in Taiwan. Overall, the patient was in good condition before the episode. 4, 5 Our observation extends the potential range of the tuberculin skin test results to include severe bulla formation and full-thickness necrosis of the overlying skin. There are few reports of acute allergic reactions to PPD. Individuals who have been exposed to M tuberculosis may occasionally experience sizable reactions, which may cause arm swelling and discomfort. 1, 3 The higher the risk a person has for developing active tuberculosis, the smaller the diameter criterion used for defining positivity in a tuberculin skin test result.Ĭomplications of the tuberculin skin test are usually mild: pain or irritation at the injection site immediately after injection. Based on the sensitivity and specificity of the PPD tuberculin skin test and the prevalence of tuberculosis in different groups, 3 cutoff points have been recommended for defining a positive tuberculin reaction: greater than 5 mm, greater than 10 mm, and greater than 15 mm of indurations. 
1, 2 The result is read between 48 and 72 hours after injection, measuring the induration diameter transversely to the long axis of the forearm in millimeters. The test is carried out by injecting intradermally into the forearm a PPD, which represents a mixture of the material produced by M tuberculosis as it is growing (Mantoux method). This phenomenon is classic for type IV delayed hypersensitivity reactions characterized by delayed course and marked induration. Lymphokines are then released, resulting in induration and erythema. In subjects exposed to M tuberculosis, T cells sensitized by the organism are recruited to the tuberculin skin injection site. 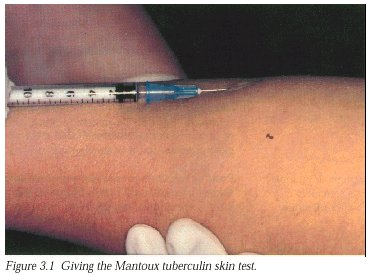
The tuberculin skin test is used for aiding in the diagnosis of active or latent M tuberculosis infection. The red discoloration of the neoskin faded away at 90 days ( Figure, E). At 30 days after inoculation, new skin had reepithelialized the entire skin defect ( Figure, D). Regrowth of the defected skin was noted 3 weeks later. The skin defect remained and was cared for with daily cleansing with normal saline, disinfected with an iodine solution (povidone-iodine), and covered with a hydrocolloid dressing (DuoDerm Convatec, Princeton, NJ). The erythema subsided spontaneously and gradually in the following days, resolving totally in 1 week. Pictures were taken serially at days 4 (A and B), 7 (C), 30 (D), and 90 (E) after the tuberculin injection. Skin ulceration over right volar forearm in a 10-year-old girl with cervical Mycobacterium tuberculosis lymphadenitis. Several tiny cervical lymph nodes remained palpable. The patient was treated with isoniazid, rifampin, ethambutol hydrochloride, and pyrazinamide for 2 months followed by isoniazid and rifampin for an additional 4 months. 
A biopsy specimen of the right cervical lesions revealed granulomatous inflammation, caseous necrosis, multinuclear giant cells, and acid-fast bacilli suggestive of mycobacterial infection. Cultures of blood and swab tests from the base of the bulla were negative for microorganisms. Vancomycin hydrochloride was administered empirically for 2 days to treat presumed cellulitis. 
The full thickness of the skin covering the bulla dislodged 2 days later, with granulation tissue and some yellowish eschar left ( Figure, C on day 7 postinjection). The erythema extended, covering almost all the volar forearm, from the elbow down to the wrist (black mark in Figure, A). The skin necrosis was related to tuberculin skin testing.Ī bulla (22 mm in diameter) developed 4 days after a PPD injection ( Figure, A and B). The patient's primary diagnosis was lymphadenitis caused by Mycobacterium tuberculosis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
